New data indicate that the global annual prevalence of pressure ulcers in SCI-persons is 32.4% (Shiferaw et al. 2020).
When a pressure ulcer is severe and not treated aggressively it can lead to further disability (e.g., reduced mobility, dependence, surgical intervention, amputation, fatal infection; Krause 1998). It has been estimated that 7-8% of those who develop pressure ulcers will die from related complications (Richards et al. 2004).
It has been estimated that pressure ulcers account for approximately one-fourth of the cost of care for individuals with SCI. In the United States alone, it has been estimated that the cost of care for pressure ulcers is about 1.2 to 1.3 billion dollars annually while prevention could cost about one-tenth of this amount (Bogie et al. 2000; Byrne et al. 1996). Because of the costs associated with treating pressure ulcers, Krause et al. (2001) state, “they [pressure ulcers] have received more attention among rehabilitation and public health professionals than any other type of secondary condition associated with SCI” (p107). Despite the attention given to prevention strategies, pressure ulcers are common among individuals with SCI (Krause et al. 2001). The most recent econometric analysis of pressure ulcer resource utilization for community dwelling people with SCI identified that 62% of the cost of pressure ulcer treatment was attributable to hospital admission costs. The average monthly costs of treating SCI-patients with pressure ulcers in community care were £2,739 in 2010 values (Chan et al. 2013). Nursing costs accounted for the greatest cost amongst non-physician health care providers (Chan et al. 2013).
(Source: summary of data from Hsieh et al. 2014)
This was an open, single-arm prospective study of the effects of MPPT (Amicapsil, Amicapsil-SCI) on wounds and pressure ulcers in persons with spinal cord injury (SCI). Spinal cord injury disrupts communication between nervous and immune systems. As a consequence, SCI-persons are immune deficient and have low ability to fight wound infections. The study includes 43 wounds (20 acute and 23 chronic) and found that MPPT consistently treated wound infections. This led to reductions in odour and exudate, and to tissue regeneration, which again led to reductions in wound size and, if osteomyelitis was not present, to closure. The reduction in tissue infection removed or reduced the frequency and severity of autonomic dysreflexia and, by combining the use of MPPT with an air supply, patients could escape constant bedrest and resume an active life. MPPT was safe, including following long-term use directly on muscle and bone, and did not cause any allergic reactions. Ease-of-use of MPPT meant that patients could be responsible for treatment, thus providing maximum opportunity for self-care and independence.
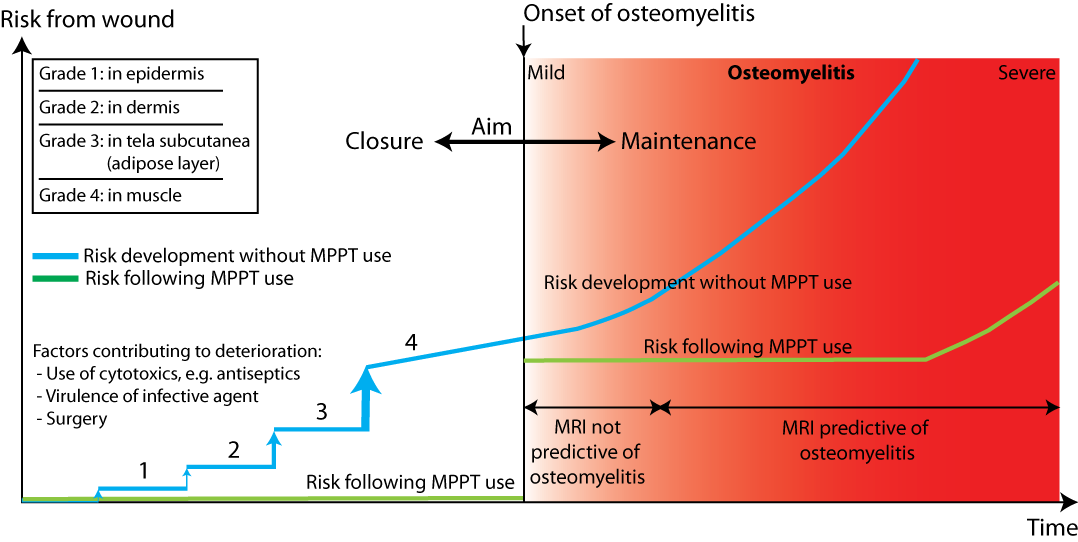
Generally in wounds, once infection has reached bone and osteomyelitis developed, the clinical picture changes completely as the bone now becomes a source of infectious debris, continuously draining into the adjacent soft tissue. This causes a diffuse and disseminated soft tissue breakdown which results in an uncontrollable wound. As osteomyelitis requires surgical removal, the aim of using MPPT changes from wound closure to improving the outcome of surgery for the patient. MPPT was able to regenerate lost tissue and to facilitate the formation of a structured and controlled fistula between the bone and the wound through which the infectious debris from the bone could drain. This substantially reduced the level of soft tissue infection and thereby the risk of septicaemia and sepsis. It also reduced the frequency and intensity of autonomic dysreflexia. Both issues are common causes of mortality. Additionally, by implementing the use of an air-providing pump, it was possible to avoid extended bedrest, allowing the patient to resume an active life while awaiting surgery, thus avoiding the detrimental effects of extended bedrest (Dittmer 1993; Teasell 1993). Finally, by minimizing the extent of soft tissue infection, less tissue will need to be removed during bone surgery. As the tissue acts as cushioning, its removal increases the risk of renewed pressure ulcers caused by protruding bones. Limiting the amount of tissue removed, will improve the long-term rehabilitation prospects for the patient.
In terms of costs, the study found:
- Acute grade 1 or 2 wounds (10 wounds): all healed and required less than 1 bottle of 750mg to heal. They usually required minimal support.
- Acute grade 3 or 4 wounds (10 wounds): Average costs of Amicapsil-SCI were £251.66. Patients were responsible for the daily dressing changes, but if daily nurse visits from start to full closure are included into the calculations at £33 per visit (NHS data), average cost per wound to closure were £56.
- Chronic grade 3 and 4 ulcers (10 ulcers 3 months to 12 years of age) without osteomyelitis: Average costs of Amicapsil-SCI to closure were £1,059.59, ranging from £359,52 to £3,954.72 with costs being affected by wound grade, age, size and individual response. For all wounds, it was the patient, family or carers, who performed the dressing changes. Study protocol required daily monitoring of the wound but once patients had become familiar with Amicapsil-SCI daily help was not needed, but could easily be reduced to every three days or less frequent. For cost calculations, daily monitoring for the first 30 days were included to teach the patient how to use Amicapsil-SCI, followed by visits every third day until closure. Using this regime, the total average cost per wound were £3,234.75.
- Chronic grade 4 wounds with osteomyelitis: Once osteomyelitis develops, the treatment goal is no longer wound closure, but to minimise risks associated with the wound until surgery. The use of Amicapsil reduces risk of sepsis, frequency and severity of autonomic dysreflexia, both of which are associated with high mortality, and improves rehabilitation outcome following surgery.
Chan et al. (2013) estimated the average annual costs of treating SCI-patients with pressure ulcers in community care were £32,868 in 2010 values and Guest et al. (2018), using the NHS THIN database, found for non-SCI persons the average costs of a grade 3 or 4 pressure ulcer for the first 12 months after presentation to the GP to be £12,845. In this study 100% of the Amicapsil-treated acute wounds closed, whereas in the findings by Guest et al. (2018) only approx. 15% healed within the first 12 months, meaning that their costs continued the following years. As these costs have not been included, the actual savings will be considerably higher. Comparing the acute grade 3 and 4 ulcers to the findings of Guest et al. (2018) the savings are 86.1% for the first 12 months only. For the chronic wounds without osteomyelitis, comparing the costs of reaching a closed wound to the costs of Chan et al. (2013) for one year, the savings are 90.2%. All of these saving-calculations only include the costs of one year, which is unrealistic as the wounds continue to deteriorate and become more and more expensive to treat.
In summary:
- Wounds without osteomyelitis: Amicapsil-SCI healed all wounds.
- Wounds with osteomyelitis: Amicapsil-SCI removed soft tissue infection and regenerated new tissue, reducing the wound to a draining fistula; this reduced the amount of tissue that needed to be removed during surgery for the osteomyelitis, which improved prospects of rehabilitation.
- Amicapsil-SCI is suitable for teletreatment, providing freedom and independence as individuals can decide themselves when and where to perform dressing changes.
- No requirement for extended or continuous bedrest, which has detrimental health consequences. All other approaches require immediate and full bedrest.
- Reduced frequency and severity of autonomic dysreflexia.
- Reduced risk of septicaemia and sepsis.
- High prevalence of pressure ulcers immediately following injury severely impact long-term rehabilitation outcomes. Access to effective treatment that ensures rapid resolution, allows timely enrolment in rehab maximising future independence.
See cases: https://willingsford.com/blog/category/wounds/sci-and-wounds/













