












100% closure rate of pressure ulcers
Download Publication
Download Publication
Download Publication
NH ( patient)
NH ( patient)
NH ( patient)
Only natural ingredients
Only natural ingredients
Only natural ingredients
VH (patient)
VH (patient)
VH (patient)
Environment and Climate Change
Climate change is caused by the combined impact of human activity on the planet. Fossil fuel is one component, but humans also release a huge amount of chemicals into the environment that affect the microbes, which to a large extent control the CO2 and N2O levels:
- The soil microbiome is responsible for around 50% of the CO2 absorption and storage and for nitrogen fixation. Changing the composition of the soil microbiome can lead to compaction, deforestation and desertification.
- The microorganisms in the oceans are responsible for more than 50% of the absorption of CO2 from the atmosphere. Again, changing the composition changes the overall equilibrium of uptake and release of gases by the microorganisms.
Therefore, if we cannot reduce the use of fossil fuel sufficiently to off-set this combined impact, it will be logical to study other factors, particularly as some of these can be reduced without any economic impact on modern society. To make an analogy if you build flood-defences, you do many different things to protect an area – you do not just build high walls or buy lots of sandbags.
A group of chemicals that strongly impact CO2 and N2O levels are antimicrobials, i.e. chemicals that kill bacteria, fungi and other microorganisms. These organisms are primary responsible for the absorption and storage of CO2 and N2O on earth and killing them will impact the ability of earth to tolerate human activity. Also, most of these chemicals are completely unnecessary and sometimes even damaging to us – so this would be a very easy and logical place to start.
MPPT itself is directly biologically recyclable, its use only requires tap-water and cotton, all packaging is recyclable, and patients or their carers can perform the dressing changes, thus eliminating the need for transport. The environmental impact is therefore minimal compared to standard care.
Further Reading
Antimicrobials’ impact on the Environment and Climate Change
Microbiomes
A microbiome is an ecosystem of all sorts of microbes that live in synergy, dividing tasks and depending on each other. Among other organisms, microbiomes consist of bacteria, funguses, viruses, and mites.
Everything on Earth is covered in a microbiome. Every single surface has its own: the ocean, the whale, the river, the fish, the lake, the air, clouds, the soil, the trunk and leaves of a tree, the worm, the beetle, the tortoise, the mouse, the deer, the dog, the human skin, the wall, the table….
Each microbiome is different in composition according to the surface it lives on and in, and it changes constantly according to changes in its micro-environment, e.g. temperature, humidity, available sources of nutrition, acidity, hormones, light intensity/direct sunlight, darkness…
Microbiomes keep the living surfaces where they live healthy and functional. They are an integral part of each living surface.
If the microbiome is altered too much or too violently, the surface sickens and, in severe cases, subsequently dies.
A microbiome is not limited to a population living strictly on top of the surface; they usually extend well into the underlying mass, without forming a well-defined border. An example is the human skin, where different microbes thrive at different depths, according to the conditions preferred by each microbial species – for example the availability of more, or less, air.
A more radical example is the soil. Here the microbiome forms an integral part of the entire space, with the microbial population changing in accordance with the varying conditions at each depth. Other examples of microbiomes forming an integral part of the entire space are lakes, rivers, the atmosphere, clouds, oceans…
All microbiomes alter according to local changes in circumstances. Examples are correlating with distance/depth from surface, changes in light, nutrition, gas availability, temperature, humidity, etc.
Antimicrobials
Antimicrobials are antibiotics and disinfectants under one name. They are poisonous chemicals that kill microbes.
Antimicrobial resistance occurs when microbes develop the ability to tolerate very high doses of antimicrobials.
Some microbes possess the ability to tolerate certain antimicrobials and they can upscale this ability very quickly. They can also quickly develop further tolerance to other types of antimicrobials. Importantly, they can donate and share such tolerances with other microbes, including between species – so that many other species acquire tolerance.
Such development of high tolerance is usually associated with increased virulence – in effect making the microbes stronger and more dangerous.
When an antimicrobial is applied, the microbes will die where it touches, and only the resistant species that tolerate the antimicrobial chemical will survive and remain. This leaves areas bare… and exposed for potential settlement by passing inherently dangerous species.
The resistant species will also use this advantage and quickly expand its territory, leaving less space for the great variety of original species of the microbiome to repopulate the area and restore a balanced, healthy, symbiotic microbial ecosystem.
As a result, the combination of the myriad of microbial species that co-existed in the original microbiome has been altered.
With the shift in composition of the microbial population, the overall use of resources available in the vicinity, from which the microbes drink, eat and breathe, will also change. Resources will be used in different proportions to how they were utilised previously by the original microbiome/microbial ecosystem. With tolerant/resistant species now in abundance and other species extinct, some resources will become superfluous while other resources will be exhausted.
There will be a consequent change in the proportion of the products generated and excreted by the microbes during metabolism. That will directly affect other organisms which use and may depend on them.
This new scenario, of certain resources rapidly being used up while others are left nearly untouched, results in a severe imbalance and disruption of the entire ecological system. The system fully depends on the release, absorption and retention of certain gases, moisture, and particular nutrients in the right amounts, and at the right pace, in accordance with the seasons.
The change in composition of microbial ecosystems therefore significantly reduces biodiversity at the microbial level. This means the disruption of the fundamental beginning of every food chain and ecosystem on Earth, causing reduced biodiversity at any and all higher levels.
Any microbe
Natural microbiome – diverse and balanced

Immediately after exposure to antimicrobials
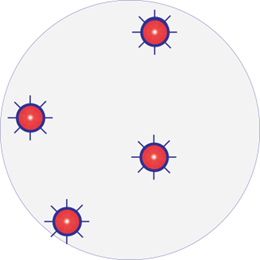
A few hours following antimicrobial exposure
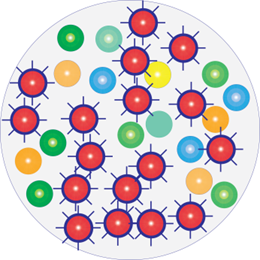
Antimicrobials in the water and soil change the composition of the river-lake-sea-ocean-floor/water/soil microbiomes and thereby shift the microbiome’s ability to capture and retain CO2. It furthermore changes the nitrogen cycle and soil structure causing desertification, deforestation and landslides – along with lots of other issues.
For simplicity reasons, only bacteria are used in the example. Antimicrobials affect all single-cell organisms and therefore the entire microbiome.
Microbes travel
Microbes are evaporated in aerosols [water droplets] and form natural microbiomes as part of the atmosphere and of the clouds – some even reach into the stratosphere. They travel with the wind and the clouds.
Different microbial species respond differently to the cold, and changing their composition and proportions means changing the formation of precipitation: whether it will fall as rain, snow or hail. It can bring about thundersnow, heavy droplet formation with hail, or torrential rainfalls, leading to erosion and landslides.
Microbial response also influences the amounts of water that will be released in different geographical locations, leading precipitation to bypass certain areas depriving them of water and causing drought and desertification.
With precipitation, the microbes travel back to Earth where they settle in a new location
Everything living on Earth – plants and animals – require carbon and nitrogen.
Both carbon and nitrogen are essential to life on Earth and readily available in the atmosphere. Actually, they are so abundant that we humans are currently blaming these gases for causing climate change. The paradox is that we also claim to be short of nitrogen.
The trouble is that animals cannot take the carbon and nitrogen directly from the gas in the air around us. First, we need the microbes to change the chemical structures of the gases.
But not just any microbe can perform these tasks. Only specific species in the soil and in the waters/oceans are capable of it; and several species are required – in the correct order.
If we alter their microbiomes or even kill key species within them, these tasks will be greatly diminished or indeed not be carried out at all.
The soil and ocean floor die away, and their structure will change from a porous air-filled sponge to a lifeless compact brick in which no animals can live, and plant roots cannot penetrate to gain a foothold. The exhausted upper soil and sea floor erode causing deforestation, leaving behind deserts of non-fertile land and ocean beds. There will be no organisms to catch the carbon and hold on to it, or to convert the nitrogen at the right pace.
Currently, the soil microbiome is responsible for around 50% of the CO2 absorption and storage as well as for nitrogen fixation; the microorganisms in the oceans are responsible for more than 50% of the absorption of CO2 from the atmosphere. It is consequently crucial to maintain healthy microbiomes.
This demonstrates that it is essential to restore the equilibrium of the innumerable, intertwined, microbial ecosystems. No human is able to understand the extent and long-term consequences of altering even a few.
The first and critical step is to stop killing the microbes by using antimicrobials unnecessarily.
Antimicrobials travel
Approximately half of all antibiotics are not removed before water is released back into nature from water treatment plants, and disinfectants [antiseptics] normally end up in landfills with general waste.
Antimicrobials are stable chemicals. They persist in soil and water, and travel in moving water, as well as on the creatures that they pass.
As surface water evaporates and forms clouds, the antimicrobial chemicals evaporate with it. This changes the microbiome of the very air that we breathe and of every cloud.
Through the air and within the clouds, the poisonous antimicrobial chemicals are carried near and far before they are released in rain over ever new areas of the Earth, where they start a renewed cycle of microbial genocide, with devastating consequences.
Antimicrobials travel
Antimicrobials are unparalleled life savers when used correctly and purposefully in medicine – human and animal – to fight a specific pathogen.
However, every year, worldwide, 13,000 tonnes of antimicrobials are used and disposed of in wound care alone – without providing any proven clinical benefit.
Antimicrobials are used with no benefit in numerous everyday household consumables. Examples include soaps, shampoos, general home cleaning products, washing detergents, hand sanitizers, clothing, toothpaste, mouthwash, face and body moisturisers, make-up, emollients, baby-wipes, baby sprays, swaddling blankets, paint, bathmats, towels etc…
As explained, the microorganisms and the microbiome underpin all things living. All higher organisms, including us, build and depend upon them. Without preserving the health of the microbial system, nature and our basis for living will collapse. Accordingly, urgent steps need to be taken to regulate and approve the use of antiseptics and antibiotics as controlled substances.
Why we MUST stop using antimicrobials in wound care immediately
In the UK there are annually 4.6 million wounds of which only approximately 60% close within the first year and many remain open for years ending out requiring limb amputation or causing sepsis. Wounds annually require 484 million wound dressing changes in UK primary care. The vast majority of dressings contain antiseptics, e.g. silver, PHMB, Octenidine, Chlorhexidine, iodine and others. In addition, many wounds are treated with systemic antibiotics (approx. 208 tonnes of antibiotics are used annually in the UK against wounds alone).
The mentioned dressing changes are limited to those in community care where the waste is typically disposed of as household waste and the antimicrobial compounds get into rivers, e.g. the Thames, via waste and leaks from water treatment plants, where the leak recently was estimated at around 50%. Antimicrobial resistance is found in the Ganges hundreds of miles before reaching human settlements; this exemplifies that microbiomes change rapidly and that the changes travel fast.
In society, there could potentially be an argument whether this devastation is worthwhile given that it saves lives. However, it does not save lives; it is used to no avail. Already back in 2016, both the US FDA and the UK NICE, independently of each other, concluded that the use of antibiotics and antiseptics in wound care does not help against a wound infection and does not support wound healing.
Unfortunately, this knowledge has led to no change in the treatment regime of wounds and ulcers meaning that these vast amounts of antimicrobials continue to be released into our ecosystem without providing any sort of benefit in its wake.
The numbers cited here cover the UK alone (2019). Practically the entire world has a comparable prevalence of wounds within its populations and they use similar approaches to treat these. Europe and North America accounts for 8.5 billion dressing changes annually, India 10.6 billion and China 10.7 billion.
| UK | 2012 | 2015 | 2020 | 2025 | 2030 | 2035 |
| Total Wounds (million) | 2.2 | 3.0 | 5.1 | 8.6 | 14.5 | 24.5 |
| Direct costs (billion £) | 5.3 | 6.7 | 9.9 | 14.6 | 21.6 | 31.9 |
| Dressing changes (million) | 233 | 319 | 537 | 905 | 1,525 | 2,570 |
| Waste (tonnes) | 18,648 | 25,504 | 42,975 | 72,415 | 122,024 | 205,618 |
| Cost of wounds (billion £) | 17.3 | 21.9 | 32.3 | 47.7 | 70.5 | 104.2 |
| *2012 prices |
